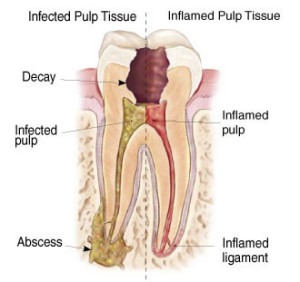
 Dental infections, i.e. dental caries, tooth decay or cavities, are bacterial in origin and cause demineralization and destruction of the hard tissues (enamel, dentin and cementum). Usually, they wreak havoc by producing acid by bacterial fermentation of the food debris that accumulates on the surface of the tooth.
Dental infections, i.e. dental caries, tooth decay or cavities, are bacterial in origin and cause demineralization and destruction of the hard tissues (enamel, dentin and cementum). Usually, they wreak havoc by producing acid by bacterial fermentation of the food debris that accumulates on the surface of the tooth.
When demineralization exceeds saliva and other remineralization factors such as those from calcium and fluoridated toothpastes, these hard tissues of the tooth progressively decay and produce dental cavities (holes in the teeth).
The mutans streptococci are mainly responsible for dental cavities. If left untreated, cavities can lead to pain, tooth loss, and dental infections. Even with all the advancements of medicine, caries are still one of the most common diseases worldwide.
While caries may vary widely in presentation, the risk factors and stages of development are similar for all cases. At first it may appear as a small chalky area, which may eventually become a large cavitation. In other cases, caries may be directly visible. For less visible areas of teeth, however, X-Rays and other methods of detection are used to find theh cavity and assess the extent of the tooth damage.
Tooth decay disease, meanwhile, is caused by certain types of bacteria that produce acid when combined with fermentable carbohydrates such as sucrose, fructose and glucose. A tooth is primarily made of minerals, and there is a constant jugglingling between demineralization and remineralization states between the tooth and surrounding saliva. People with little saliva are particularly prone to developing caries and dental infections.
When the pH at the surface of the tooth goes below 5.5, it means that demineralization occurs at a faster rate than remineralization. This means there is a net loss of mineral structure on the surface of the tooth. As most foods are acidic, a lack of proper remineralization leads to tooth decay. Dental organizations recommend various preventive and prophylactic measures such as proper oral hygiene and dietary changes to avoit dental infections.
Signs and Symptoms of Dental Infections
Not all individuals experiencing dental caries are aware of the disease. The earliest sign of a new cavity is the appearance of a small chalky area on the surface of the tooth, revealing an area of demineralization of enamel. This early sign is called a “microcavity” or incipient carious lesion. As the area keeps demineralizing, it can turn brown and eventually develop into a cavity. The process is reversible until the cavity forms, but once it does the lost tooth structure can no longer regenerate. A brown and shiny lesion indicates the tooth once experienced dental caries but the demineralization process stopped, leaving a stain. A brown spot dull in appearance, meanwhile, suggests there are active caries.
The cavity becomes increasingly more visible as the enamel and dentin in the tooth are destroyed. The affected areas gradually change colors and become soft to the touch instead of strong. Once the decay passes through enamel, the dental tubules become exposed and lead too toothache, as these dental tubules have passages to the nerve(s) of the tooth. In such cases, the pain may get worse with exposure to cold, heat or sweet foods and drinks. Dental infections can also cause bad breath and foul tastes.
Causes of Dental Infections
The carries process does not develop the same for all individuals. Different people are susceptible to different degrees, depending on the shape of their teeth, their oral hygiene habits and the buffering capacity of their saliva. Dental caries can affect any surface of the tooth that is exposed to the oral cavity, but it cannot affect the structures retained within the bone. All caries occur from acid demineralization with higher rates than saliva and fluoride remineralization. Nealry all acid demineralization occurs where food is left on teeth. Most food is left between teeth, which in turn results in 80 percent of cavities occurring inside pits and fissures on chewing surfaces where fluoride, brishing and saliva cannot properly reach to remineralize the tooth.
Diagnosing Dental Infections
For a primary diagnosis, dentists inspect all visible surfaces of the teeth using a good light source, dental mirror and explorer. Dental X-rays can show dental caries before they are otherwise visible, particularly when it comes to caries between the teeth. Large dental caries are often visible to the naked eye, but smaller ones may be difficult to spot. Dentists also frequently resort to visual and tactical inspection in addition to X-rays to diagnose pit and fissure caries. Early caries that has not yet cavitated is often diagnosed by blowing air across the suspect surface. This move removes moisture and changes the optical properties of the unmineralized enamel.
As previously mentioned, the carious process can be reversed if the cavity is not yet present. The caries may be treated with fluoride and the tooth surface remineralized. Once the cavity sets in, a restoration will be necessary to replace the lost tooth structure. Caries can be classified by etiology, location, rate of progression, and affected hard tissues.
How to Prevent Dental Infections
The most important aspect in preventing dental infections is personal oral hygiene, which consists of proper brushing and flossing at least once a day. Oral hygiene aims to minimize any etiologic agents of disease in the mouth, while the purpose of brushing and flossing is to remove and prevent the formation of plaque, which mostly consists of bacteria.
As bacterial plaque builds up, the tooth becomes increasingly vulnerable to dental caries when carbohydrates in the food are left on teeth after a meal or a snack. A toothbrush can remove plaque o accessible surfaces, but it cannot reach between the teeth or inside pits and fissures on chewing surfaces. When used appropriately, dental floss can remove plaque from areas that could otherwise develop proximal caries. Interdental brushes, water picks and mouthwashes may also prove useful.
Professional hygiene care implies regular dental examinations and cleanings, completely removing plaque. Dental X-rays taken at regular dental visits can also help detect caries development early on, which might make things a whole lot easier.
In terms of dietary changes, the frequency of sugar intake is actually more important than the amount of sugar consumed. Bacteria in the mouth produce acids that can demineralize enamel, dentin and cementum in the presence of sugar and other carbohydrates. The more an individual exposes their teeth to such environment, the more likely they are to develop dental caries. Minimizing snack frequency can be of great help, as snacking creates a constant, continuous supply of nutrition for bacteria in the mouth, allowing it to thrive. Sticky and chewy foods such as dried fruit or candy also tend to stay on teeth longer and should be eaten as part of the meal, after which brushing is indicated.
Calcium found in various products such as milk and green vegetables is also recommended to protect against dental infections, while special calcium and fluoride supplements can decrease the incidence of dental caries. A fluoride toothpaste or mouthwash can prove helpful.
Tooth Infections on a Global Scale
Roughly 2.43 billion people worldwide, i.e. 36 percent of the world’s population, have dental caries in their permanent teeth. This issue is most prevalent in countries in Latin America, Middle East countries, and least prevalent in China. In the U.S., dental caries make the most common childhood disease, with five times greater pevalence than asthma. The number of cases is decreasing in some developed countries, a drop generally attributed to better oral hygiene practices and proper preventive measures such as fluoride treatment.
1 comment
What’s upp to every , because I am actually keeen of reading this web site’s post
to be updated daily. It consists of nice material.
Comments are closed.